Blog
What you need to know about physiotherapy and podiatry.




Written by
Senior Partner & Principal Physiotherapist at Women And Children Centre and Physio & Sole Clinic
Farha is a physiotherapist who specialises in musculoskeletal care for infants, children, adolescents, and women. She has a strong interest in scoliosis management, paediatric conditions, and supporting women through pregnancy and postnatal recovery through personalised, evidence-based rehabilitation.
Pelvic girdle pain (PGP) is pain around the sacroiliac joints, pubic bone, hips, or lower back that can persist as back pain after delivery. It is common during pregnancy and may continue postpartum. While many women improve within a few weeks, symptoms can last for months without proper rehabilitation.
In This Article
As a physiotherapist working with women in Singapore, one of the most common things I hear from new mothers is this:
“I thought the pain would go away after the baby was out… but my lower back and pelvis still hurt.”
If you’re experiencing pelvic girdle pain after giving birth, you are not alone.
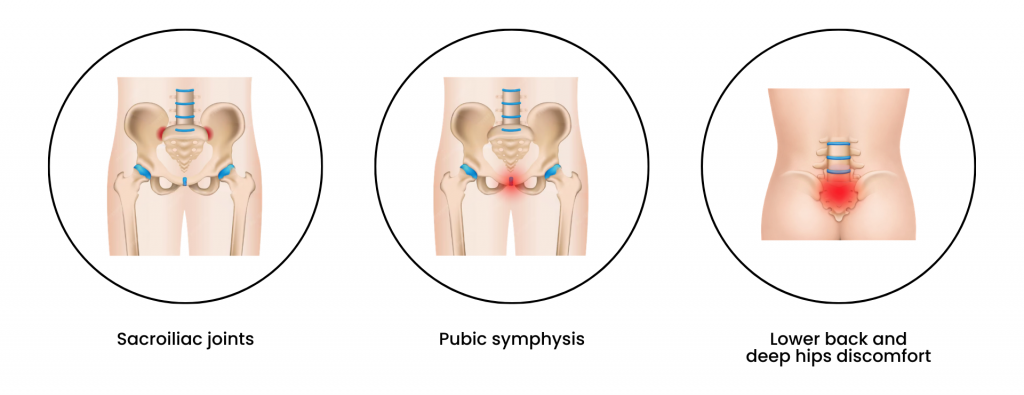
Pelvic girdle pain refers to discomfort around:
It can feel sharp, aching, stabbing, or like instability — especially when:
Many women describe it as persistent back pain after delivery, or say they’re searching desperately for “after pregnancy back pain relief.”
Here’s what’s important to understand: pregnancy and childbirth place enormous stress on the pelvis. Hormones like relaxin soften ligaments. Muscles stretch. The abdominal wall changes. The pelvic floor is loaded for months. Delivery — whether vaginal or C-section — is a major musculoskeletal event.
Your body does not “reset” the moment your baby is born.
Most cases involve a combination of:
PGP is rarely caused by one isolated issue.
That’s why generic exercises often fail — rehabilitation must address the root cause.

It can be — but persistent pelvic girdle pain should not be dismissed.
Most women improve within the first 6 weeks postpartum as hormones settle. However, research suggests that approximately 1 in 10 women may experience symptoms beyond three months if not treated appropriately.
In Singapore, many mothers:
When core and pelvic muscles haven’t regained coordination, the pelvis remains mechanically stressed. Over time, pain shifts from hormone-related to movement-related.
Persistent pelvic girdle pain is often a sign that the body needs structured rehabilitation — not just time.

This is extremely common.
In the early postpartum period, activity levels are relatively low. As you:
The load on the pelvis increases.
If deep stabilising muscles — particularly the transversus abdominis, glutes, and pelvic floor — are not functioning optimally, the pelvic joints absorb uneven forces.
Activity is not the problem. Unprepared load is.
Pain flare-ups often signal that progression was too fast, not that exercise is harmful.

Here are evidence-based strategies I recommend to mothers:
1. Modify Daily Movements
Reducing repetitive joint stress accelerates recovery.
2. Progress Impact Gradually
If symptoms flare, reduce load and rebuild gradually.
5. Address the Pelvic Floor
Pelvic floor dysfunction may present as:
Proper assessment determines whether muscles are weak, tight, or poorly coordinated.
Even if your symptoms seem “mild,” I strongly encourage mothers to seek assessment from a physiotherapist or pelvic health therapist. Many women assume they just need to wait it out, but persistent pelvic girdle pain after childbirth can become harder to resolve the longer it is left untreated. A professional assessment ensures that you are exercising safely, progressing at the right pace, and not unknowingly reinforcing compensatory movement patterns that keep the pain going.

Seek professional assessment if:
In Singapore, you can directly consult a physiotherapist without GP referral in private practice. Early intervention shortens recovery time and prevents chronic pain patterns.

At Women & Children’s Centre, our physiotherapists take a comprehensive approach to postpartum pelvic girdle pain. We understand that recovery is not just about doing exercises — it’s about restoring confidence, stability, and comfort in your body.
During your session, we assess:
Beyond prescribing exercises, treatment may include:
Our goal is not just short-term after pregnancy back pain relief, but long-term pelvic resilience. With the right assessment and treatment plan, most mothers see significant improvement within weeks and regain confidence in movement.
Pelvic girdle pain after childbirth is common — but persistent pgp pain is treatable.
If you are unsure whether what you’re experiencing is “normal,” that uncertainty alone is reason enough to seek guidance. Early intervention is always easier than correcting long-standing pain patterns.
Phone: 9126 8257
Fax: 6281 1209
Email: contact@physioandsole.com
Whatsapp a Podiatrist: 87706213